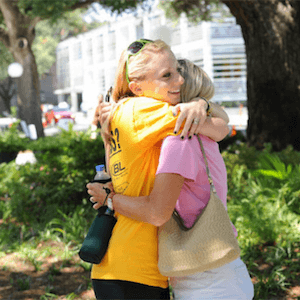
1. Get an epinephrine auto-injector.
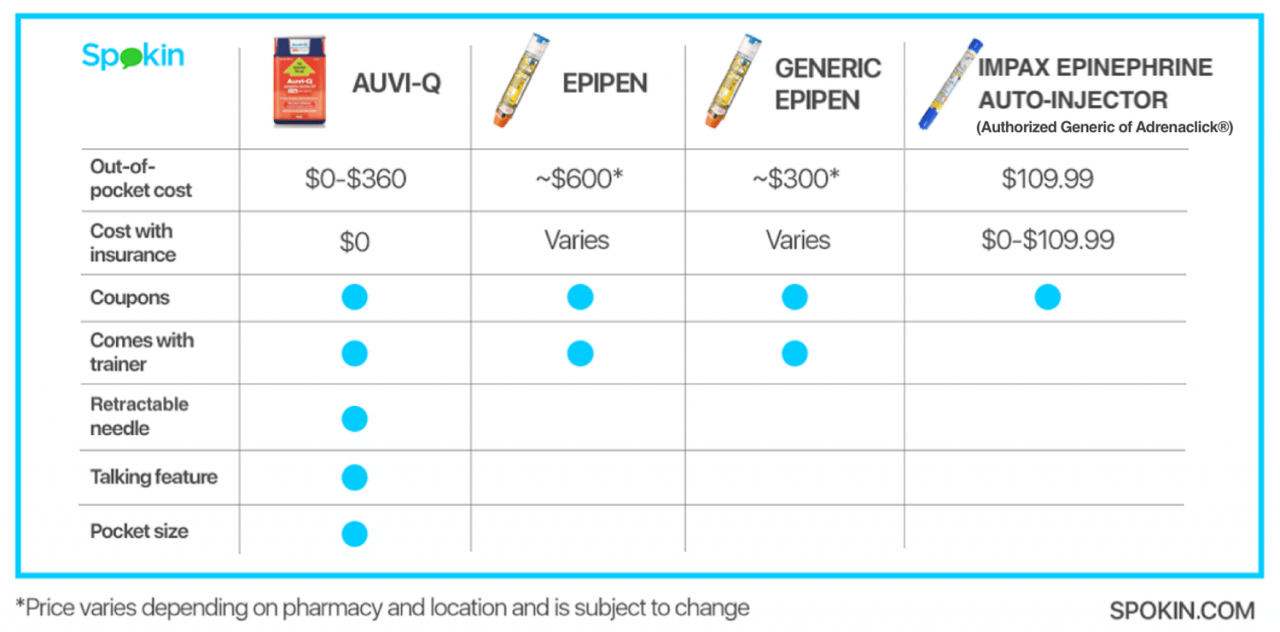
If you suspect your child has a food allergy, call your pediatrician ASAP. Your child’s doctor can call in a prescription for an epinephrine auto-injector and refer you to an allergist without an office visit. Our auto-injector comparison chart (pictured right) can help you find the best option for you. Also, read up on the newest option on the market and How to Get AUVI-Q for $0.
Since it could take weeks or months to get an appointment with an allergist, fill the prescription right away. Be sure to keep two with you at all times in case one malfunctions or a second dose is required. Remember that even if your child’s initial reaction was mild, it could be more severe the next time.

2. Know how to use your auto-injector.
A parent is the first line of defense when there’s an allergic reaction, so even if needles make you queasy, you need to get comfortable using an auto-injector. Spokin’s auto-injector how-to videos are great 60-second tutorials that show the exact steps for using an auto-injector. Videos are available in English, Spanish and Chinese.
Most auto-injectors come with a “trainer” that you can use for practice. Or if you or someone you know has an expired auto-injector, inject it into an orange to get a feel for how much pressure is needed.
3. Find an allergist.
Allergists are specialists who can offer guidance on managing food allergies and should be aware of the latest research, treatments and therapies. To find the best of the best, get a referral from your pediatrician or ask parents of other food allergic children for a recommendation – they are your most valuable resources. If you live in the Chicago area, check out this list of the Top 7 User-Rated Allergists.

4. Learn how to read a food label.
It’s not as easy as it sounds. Obviously, your child needs to avoid foods that contain his or her allergens, but don’t forget about foods that may accidentally contain the allergen, commonly referred to as cross contamination or cross contact. Packaged foods are required by law to list an allergen in plain English if it’s an ingredient, but only if it’s one of the top 8 most common allergens (milk, eggs, peanuts, tree nuts, fish, shellfish, soy or wheat). Check out this complete how-to guide.

5. Decide how to handle the allergen at home.
It is important to remember there is no one right way to manage allergens in your home- it is a matter of preference. Some families make the home a completely allergen-free zone, while others find safe ways to keep it in the house for themselves or siblings without food allergies. Storing allergens can also vary depending on the severity of the allergy. Talk with your doctor and other food allergy parents to figure out what’s best for your family.
6. Know the symptoms of a reaction and how to treat them.
Every allergic reaction can look – and feel – a little different. The symptoms range from mild to severe, and in the worst cases, a child can experience anaphylaxis. If your child exhibits one mild symptom – like hives, vomiting, sneezing or diarrhea – you can give him or her a dose of Benadryl (check with your pediatrician for proper dosage). When two or more mild symptoms present themselves, administer the auto-injector and call 911. If your child has one severe symptom like trouble swallowing, wheezing, chest pain or a weak pulse, you should also use the auto-injector and call 911. Get advice from an allergist and learn how to prepare for an emergency.

7. Learn how to order in a restaurant.
Even if it seems overwhelming and impossible at first, dining out is totally doable if you plan ahead. Take the time to check out a restaurant’s menu in advance – most are available online – and give them a call to assess if they’re food allergy-friendly. Start with a few questions: “Do you have experience catering to guests with food allergies? Have you been successful serving customers with [insert allergen]? How present is the allergen in the kitchen?” Be sure to ask what oil is used in the fryer – peanut oil is commonly used – and what gets fried together. For example, people with a shellfish allergy shouldn’t eat chicken fingers that are cooked in the same oil as fried shrimp. Also, those with nut allergies should pay close attention to the dessert menu, a hiding spot for many tree nuts.
If the restaurant can’t answer simple questions or you don’t feel comfortable, pass and pick another place to eat. Once you’re seated, make sure the waitstaff is aware of all food allergies and ask them to ensure the allergens are not in the dish your child orders. When they bring out the food, ask again. Try not to be self-conscious – your child’s health is at stake. For more details, check out our complete guide on How To Order In A Restaurant With Food Allergies.

8. Have a heart-to-heart with
your child about food allergies.
Sitting an 18-month-old down to discuss a medical diagnosis is tough, but every parent should try to find an age-appropriate way to talk about food allergies. Use clear phrases like, “This food can make you very sick,” and “You can’t eat this.” Parents can also model healthy habits by asking, “What’s in this? Is it safe for my child to eat?” when ordering at restaurants or eating at a relative’s home. Read up on the 36 skills to teach your food allergic child.